Dr Mohd Hamzah Kamarulzaman is the best cardiac surgeon in Malaysia with more than 33 years of expertise. Aortic surgery, intracardiac repair, coronary artery bypass surgery, and grafting are among his specialities. His other expertise's are Tetralogy of Fallot, Patent Foramen Ovalle, Atrial septal defect (ASD), Ventricular Septal defect (VSD), Valve Repair and Replacement. From 2001 to 2003 and 2014 to 2016, he served as the Vice President of the Malaysian Association for Thoracic and Cardiovascular Surgery (MATCVS).Currently, he works in KPJ Ampang Puteri Specialist Hospital in Ampang, Malaysia.
Dr Mohd Hamzah Kamarulzaman completed his MD and FRCS degrees from the University of Edinburgh in 1991, and he is a part of the Royal College of Surgeons of Edinburgh. He is a member of the Malaysian Board of Cardiothoracic Surgery's training committee and a CPR Committee member and instructor in Penang. He belongs to several renowned organisations, including the Malaysian Medical Association, the Malaysian Medical Relief Society, and the Malaysian Islamic Medical Association.
He has worked at a variety of hospitals, including Hospital Serdang in Malaysia, Avisena Specialist Hospital in Malaysia, and Thomson Hospital in Kota Damansara, Malaysia
Dr Mohd Hamzah Kamarulzaman has won many awards which includes :
- Life Member Malaysian Medical Association (MMA)
- Training Director Malaysian Board for Cardiothoracic Surgery
- Member of Islamic Medical Association Malaysia (IMA Malaysia)
- Life Member of Malaysian Medical Relief Society (MERCY)
- CPR Committee member and Instructor, Penang
- Vice President Malaysian Association for Thoracic and Cardiovascular Surgery (MATCVS) (2001-2003, 2014-2016)
List of treatment provided by Dr Mohd Hamzah bin Kamarulzaman:
- Neonatal and Infant cardiac surgeries
- Complex congenital heart surgeries
- Coronary Artery Surgery
- heart disease
- Balloon Septostomy
- Pulmonary and Mitral
- Valve Repair Replacement
- Atrial Fibrillation Surgery
- Ross Procedure
- Cardiac Tumour Treatment
- Aortic Dissection Repair Surgery
- Minimal access surgeries for valves
- Cardiac ablation
What Is the Tetralogy of Fallot?
Your heart's primary duty is to circulate blood throughout your body. This blood carries nutrients and oxygen throughout your body. Your heart may not be effective in pumping blood to other organs if it isn't working properly. This has an impact on the amount of oxygen delivered to other body tissues. When a person is born, he or she may have cardiac abnormalities or issues. Congenital heart defects are the name for these defects. Tetralogy of Fallot (TOF) is a deadly congenital cardiac condition if it is not corrected. "Tet" is another name for it. The "tetra" in the condition's name refers to the four issues that it causes. Dr Etienne Fallot is the name of the condition.
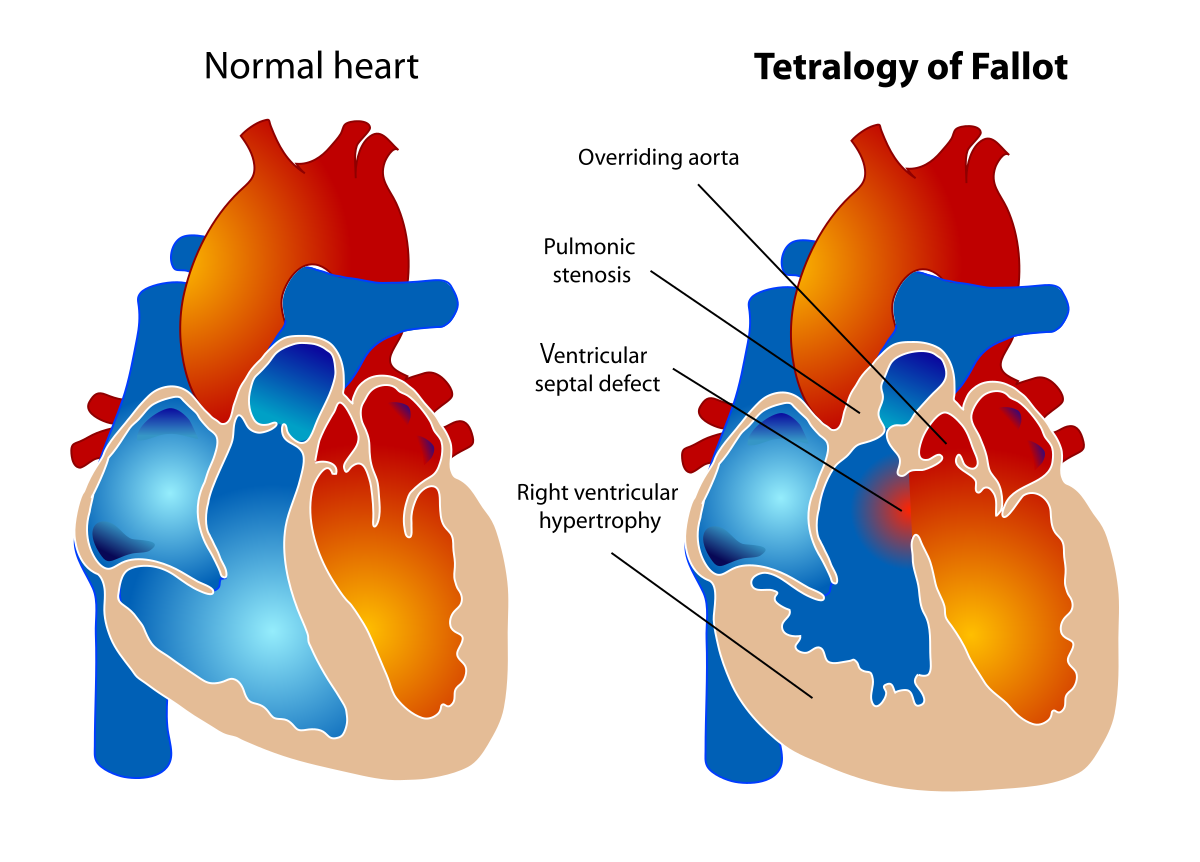
Tetralogy of Fallot (TOF) is a cardiac abnormality that refers to a group of four heart abnormalities that frequently occur simultaneously. The following are the four defects:
- Ventricular septal defect (VSD): A hole between the right and left pumping chambers of the heart is known as a ventricular septal defect (VSD).
- Overriding aorta: The aortic valve in the overriding aorta is swollen and seems to originate from both the left and right ventricles rather than the left ventricle as it does in normal hearts.
- Pulmonary stenosis: Pulmonary stenosis is a constriction of the pulmonary valve and outflow tract or region below the valve that causes blood flow from the right ventricle to the pulmonary artery to be obstructed (blocked).
- Right ventricular hypertrophy: Because the right ventricle is pumping at high pressure, the muscular walls of the right ventricle thicken.
What Are the Tetralogy of Fallot (TOF) Symptoms?
Cyanosis is a frequent symptom. Healthy newborns' skin can be blue around the mouth or eyes due to large veins beneath the skin, but their lips and tongue are pink. Blue lips and tongues, as well as bluish skin, are common in babies with low oxygen levels in the blood.
During weeping or eating, a child with TOF may have abrupt episodes of severe cyanosis known as "hypercyanotic spells" or "Tet spells." Tet spells frequently cause older children to automatically kneel, which helps to break the spell.
Other indicators include:
- tiring easily
- difficulty breathing
- heart murmur
- fussiness
- rapid heartbeat (palpitations)
- fainting
- "clubbing," where the skin or bones around the tips of fingers are widened or rounded
How Is Tetralogy of Fallot (TOF) Diagnosed?
To determine if a baby has tetralogy of Fallot and to learn more about the infant's heart and blood vessels, doctors may do a variety of tests, including.
- A pulse oximeter is a tiny sensor that attaches to your fingertip, toe, or ear and monitors the amount of oxygen in your blood. Before being sent home from many newborn nurseries, all newborns are given a pulse oximeter test to ensure that their oxygen levels are normal.
- An electrocardiogram (ECG) is a test that records the heart's electrical activity.
- chest X-ray
- An echocardiogram (echo) is a cardiac ultrasound image. It can monitor the direction and speed of blood flow as well as record the passage of blood through the heart.
- Cardiac catheterization involves inserting a thin, flexible tube called a catheter into the heart, generally through a vein in the leg or arm, to get information about the heart, blood pressure, and blood oxygen levels. Through the cardiac catheter, a device is sometimes introduced into the heart or blood arteries.
Treatment for Tetralogy of Fallot
When a kid is diagnosed with tetralogy of Fallot, the immediate focus is on establishing if the youngster's oxygen levels are within a safe range. If the child's oxygen level is severely low immediately after delivery, a prostaglandin infusion is generally started to maintain the ductus arteriosus open, allowing more pulmonary blood flow and raising the oxygen level. Surgical intervention is generally required in the newborn period for these infants. In the first week of life, most infants with normal oxygen levels or relatively moderate cyanosis are allowed to go home.
As long as the oxygen levels are acceptable, the complete repair is generally done electively when children are around 6 months old. Decreases in oxygen saturation that occur gradually or suddenly may necessitate early remedial action. The deformity must always be surgically corrected. Before the final repair, individuals may require surgical palliative treatment.
The ventricular septal defect is closed with a synthetic Dacron patch in the tetralogy of Fallot repair so that blood may flow normally from the left ventricle to the aorta. A combination of cutting away (resecting) obstructive muscle tissue in the right ventricle and expanding the outflow channel with a patch is used to enhance (enlarge) the constriction of the pulmonary valve and right ventricular outflow tract.
However, in certain infants, the coronary arteries branch across the right ventricular outflow tract, preventing the patch from being implanted. An incision in this location to implant the patch would harm the coronary artery in these newborns, thus it is not possible to do so safely. A hole is created in the front surface of the right ventricle (avoiding the coronary artery) and a conduit (tube) is stitched from the right ventricle to the bifurcation of the pulmonary arteries to enable unimpeded blood flow from the right ventricle to the lungs when this happens.
Follow-up care for TOF
The majority of adult individuals with tetralogy of Fallot had their tetralogy of Fallot corrected as children. They started as a "blue baby," but surgery has nearly always turned them pink. Some patients' surgical outcomes are good, and they have no long-term complications. Unfortunately, the majority of them have problems, the most serious of which is pulmonary valve leakage, often known as "pulmonary regurgitation." This can expand the right heart chambers, limiting physical activity as well as causing heart rhythm problems and, in rare cases, abrupt cardiac death.
Most patients with corrected tetralogy should be evaluated by a congenital heart expert regularly (typically once a year). A tissue valve replacement can be used to address pulmonary regurgitation. This is typically a low-risk treatment that allows the patient's heart to shrink again, improving their quality of life and life expectancy. In adult patients, these prosthetic pulmonary valves typically survive a long time, although they must be monitored by a physician. Fortunately, if these valves fail today, they may be changed using catheter-based valves (such as the Melody valve) rather than undergoing reoperation. Tetralogy is a hereditary disease that affects certain people. It's critical to identify this so that additional indications of their genetic defect may be properly handled.
Dr Mohd Hamzah bin Kamarulzaman is a well-known and well-reputed cardiologist with over 33 years of expertise. He has treated hundreds of patients to date, and his expertise has helped patients in improving their lives and providing them with a happy and healthy lifestyle. He currently lives in Ampang, Kuala Lumpur, Malaysia, and is associated with KPJ Ampang Puteri Specialist Hospital, Ampang, which is one of Malaysia's top hospitals.